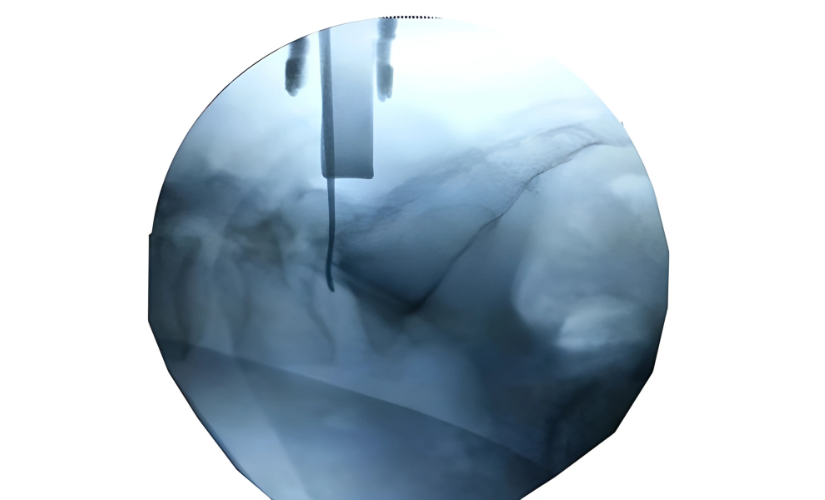
Lumbar Prolapsed Disc
Surgical Approach and Recovery
The standard surgery for disc prolapse is microdiscectomy or endoscopic discectomy. The herniated disc material is removed through a small incision, using specialized instruments that limit muscle and bone injury. This technique is safe, causes minimal scarring, and offers rapid relief from leg pain. Patients typically recover in 1-2 weeks but are advised to avoid heavy lifting, twisting, and prolonged sitting to prevent recurrence.
Frequently asked questions
Surgery is considered if a patient has severe, persistent pain, muscle weakness, sensory/motor loss, or if the disc has migrated out of position.
Microdiscectomy or endoscopic discectomy is done under general anesthesia through a 2-2.5 cm incision using an endoscope or operating microscope to remove disc material and relieve nerve pressure.
Most are discharged within 48 hours; pain relief is rapid, and normal activities can be resumed in 1-2 weeks, provided spine-protective precautions are followed.
Yes. These areRare risks include infection or recurrence. Lifelong care—avoiding heavy lifting and maintaining good posture—is essential. vital for destroying residual cancer cells and reducing the risk of recurrence, and are tailored to each patient.
Many patients improve with physiotherapy and medication alone; surgery is for those who don’t respond or have neurological deficits.